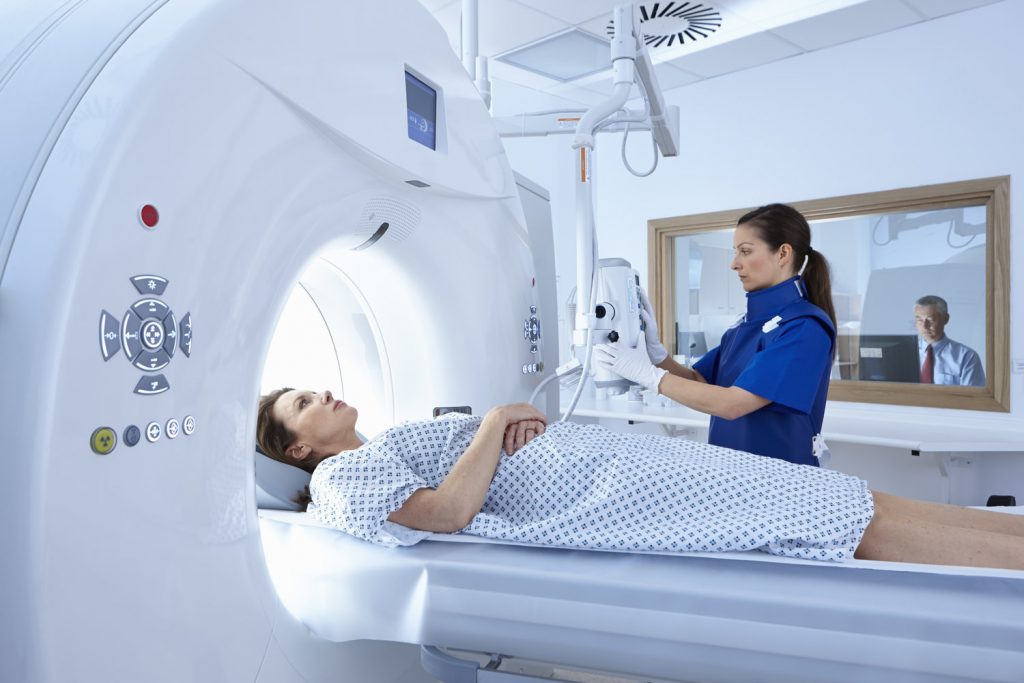
My mother was experiencing mild symptoms of viral infection. Immediately I took her to the hospital, where the doctor conducted several blood tests. Though the results were absolutely normal, he further advised performing an HRCT scan to diagnose COVID-19.
HRCT or High-resolution computerized tomography scanning uses X-rays to produce detailed images of the inside of your body. These images show cross-sections (slices) through the heart and lungs. Today, health care providers trying to use imaging tests to diagnose COVID-19.
HRCT is used for diagnosis and assessment of interstitial lung diseases, such as pulmonary fibrosis, and other generalized lung diseases such as emphysema and bronchiectasis.
The HRCT scanning helps to diagnose the area of involvement if the infection is present inside the chest region. The scores range from 0 to 5 which means;
- 0 – No involvement
- 1 – Up to 5%
- 2 – 6 to 25%
- 3 – 26 to 50%
- 4 – 51 to 75%
- 5 – >76%
Must read l How do you prepare before entering into a scanning room
HRCT scan and Coronavirus
The American College of Radiology (or ACR), which represents nearly 40,000 radiologists in the United States, has issued guidance that CTs and x-rays should not be used as a first-line tool to diagnose or screen for COVID-19.
Current evidence suggests that an HRCT scan and x-rays are generally not specific enough to either diagnose or rule out COVID-19 on their own.
However, when used with lab tests, medical history, and a physical exam, CT scans or x-rays can be helpful for diagnosing COVID-19 or determining the severity of the disease in some patients (1).
There are four major reasons for the ACR’s recommendation:
Reason No. 1
A chest CT or x-ray cannot accurately distinguish between COVID-19 and other respiratory infections, like seasonal flu. Unlike swab tests, which lead to specific diagnoses of COVID-19, imaging findings are not specific enough to confirm COVID-19.
They can only point to signs of an infection. Those signs could be due to other causes, including seasonal flu which is very common at certain times of the year.
Reason No. 2
A significant percentage of patients with COVID-19 have normal chest CTs or x-rays. For those patients, a normal imaging result could falsely convince them that they are healthy. If they believe they are healthy, they are at greater risk of spreading the virus to others.
Reason No. 3
Because COVID-19 is highly contagious, using imaging equipment on COVID-19 patients is a serious hazard for healthcare providers and other patients.
Must read l Know the difference between CT scan and MRI
CT scanners are large and complex pieces of machinery. They need to be thoroughly cleaned between each potential COVID-19 patient. But even with careful cleaning, there is a risk that the virus could remain on a surface in a CT scanner room.
Additionally, moving potential COVID-19 patients to and from a CT scanner room increases the risk of spreading the virus inside of healthcare facilities. It also means that fewer CT scanners would be available for other vulnerable patients who need this imaging test.
Reason No. 4
While patients with COVID-19 can show an abnormality on either a chest x-ray or CT scan, many other lung problems can look very similar. Additionally, the absence of an abnormality on either a chest x-ray or CT scan does not necessarily exclude COVID-19.
For this reason, most experts and medical societies advise against the use of an imaging test alone to diagnose or rule out COVID-19.
A complementary approach
Though CT scans and x-rays aren’t recommended as the only way to diagnose COVID-19, they may be appropriate on a case-by-case basis (2).
For patients with severe symptoms, imaging might help to assess the seriousness of the disease. And when used with lab tests, a thorough medical history, and a physical exam, an HRCT scan or x-rays can be helpful for determining a plan of care for a patient.
Must read l What have been advised to do before a scan
Overall, imaging plays a complementary role in the management of patients with COVID-19. It is not recommended as a sole screening tool. Currently, laboratory tests are the most accurate method of diagnosing this disease.
The KeyNote
As I said, my mother was experiencing mild symptoms of viral infection. After the doctor’s advice, she went through an HRCT and RTPCR testing for COVID-19.
We got the report on the same day for the scan, which says my mother is free from infection. Here are the details;
- History – Fever
- No pneumothorax.
- No evidence of pleural effusion/thickening on either side.
- Trachea and major airways appear patent.
- No evidence of abnormal mediastinal/hilar lymphadenopathy.
- Normal cardiac configuration. No pericardial effusion.
- Major mediastinal vessels and aorta appear normal.
- Visualized thoracic esophagus appears collapsed, unremarkable.
- Degenerative changes in the spine. No focal lesion.
| LOBES | RIGHT LOBE | LEFT LOBE |
| Upper Lobe | 0 | 0 |
| Middle Lobe | 0 | xxx |
| Lower Lobe | 0 | 0 |
| Total | 0 out of 25 |
Though the Antigen test was negative, the RTPCR test took 6 days to come which results in POSITIVE. Immediately, the doctor started the Covid-19 medicine protocol. She is feeling better now.
Again, what I am trying to convey to you is HRCT scan alone has a limited role in diagnosing COVID-19 infection. Go and get the RTPCR test done first (I doubt the potency of the Antigen test), and perform your scan just after.